This year has been a year of unprecedented events that have caused profound changes in the way we view and carry out work, socialize, do errands, take classes, and use our downtime.
How have stay-at-home orders, the risk of infection with the coronavirus, continued racial injustice, job losses, and isolation impacted the mental health of Americans? What was the mental health status of people in the US leading up to 2020?
Here we highlight some of the most recent statistics around mental health in the US in 2020.

Report: The State of Mental Health in America
At the beginning of 2020, Mental Health America released a report that showed the state of mental health using the most recent data up to that point, disaggregated by state.
Some of the main findings of the report were as follows:
- From 2012 to 2017, the prevalence of past-year Major Depressive Episode (MDE) increased from 8.66 percent to 13.01 percent in youth ages 12-17. This signifies an increase of over one million youth.
- Between 2008 and 2017, the proportion of adolescents that experienced serious psychological distress in the last 30 days increased by 71 percent, and the proportion that seriously considered attempting suicide increased by 47 percent.
- The prevalence of any mental illness (AMI) among adults ages 18 and over increased slightly from 18.19 percent in 2012 to 18.57 percent in 2017, and suicidal ideation among adults increased from 3.77 percent in 2012 to 4.19 percent in 2017. That is equivalent to over 10.3 million adults who have serious thoughts of suicide in the US.
The findings of the report highlight the poor state of mental health in the US prior to the start of the COVID-19 pandemic.
Mental Health Response During the COVID-19 Pandemic
The data from the State of Mental Health report does not reflect the changes that have occurred as a result of COVID-19. Logically, however, with such abrupt changes to our daily lives comes adjustments in our mental state and way of life.
After months and months of keeping our guard up against the risk of the coronavirus, people have felt fear, worry, and concern, which has led to an increase in the prevalence of anxiety and depression among youth and adults. It is logical that the data above will be aggravated by the current pandemic.
To monitor the recent changes in mental health, the National Center for Health Statistics partnered with the CDC to build the Household Pulse Survey to monitor changes in mental health week to week.
The most recent CDC mental health surveillance data shows that 46.6 percent of adults 18 to 29 years old felt symptoms of anxiety or depression in the week of July 16 to July 21. This is up over 6 percent compared to the period of April 26 to May 5, when data collection for surveillance began.
One group of researchers reviewed the results of 65 studies that looked into the mental health impact of the pandemic on different populations. Researchers found that children and older people, as well as those with underlying health conditions, are likely to be experiencing worry, anxiety, and fear. Medical staff is also a population experiencing extreme physical and psychological pressure.
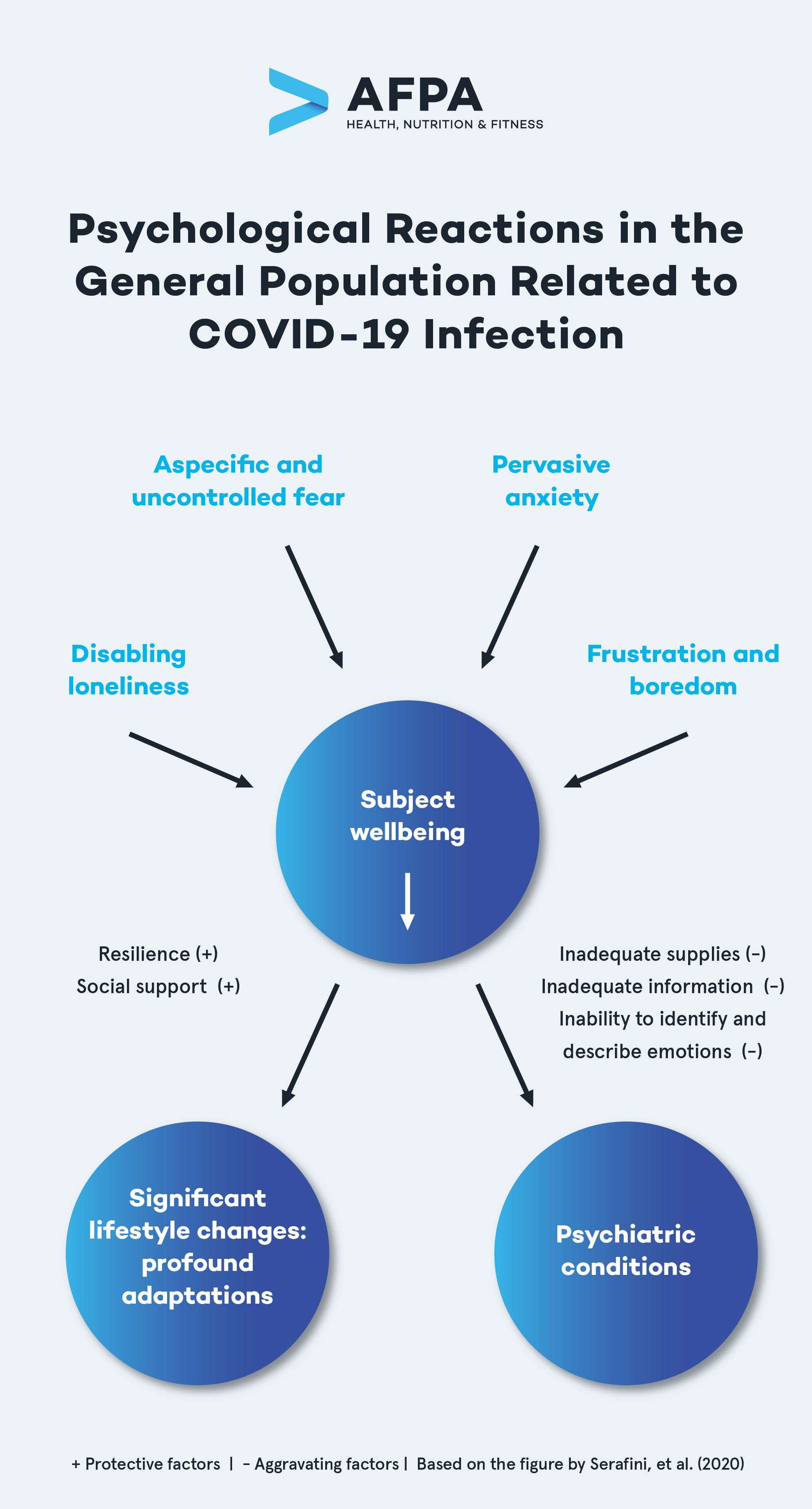
A study by Serafini and his team presents a useful summary of the most relevant psychological reactions in the general population as a result of the COVID-19 pandemic. The figure below, which comes from the study, demonstrates that there are several unifying factors that affect wellbeing and mental state, but there are also relative factors that modify people’s responses to those factors in positive and negative ways.
Resilience and social support, for example, are protective factors that help people manage the mental health effects of the pandemic, while factors like not having enough supplies, not having enough or factual information, and the inability to express what you are feeling are all factors that can make your mental health response worse.
So, even though parts of the country are beginning to loosen some of the restrictions put in place to control the spread of the coronavirus, the rates of anxiety and depression have continued to grow.
When to Refer Your Client to a Mental Health Specialist
As a health and wellness coach, your clients often confide in you to discuss many of their struggles. While the information they share with you is confidential, and you can offer tools within the limits of your practice to support them, it is important to recognize when a client’s mental health needs are out of your scope of work.
When signs of serious anxiety and depression arise, it is essential that you refer your client to a licensed mental health specialist. Some warning signs of serious anxiety and depression include:
- Feelings of helplessness and hopelessness
- A loss of interest in daily activities
- Severe appetite or weight changes
- Sleep changes, like insomnia or chronic oversleeping
- Anger or irritability
- A sudden and chronic loss of energy
- Strong feelings of worthlessness or guilt
- Substance abuse, compulsive gambling, and recklessness
- Unexplained aches and pains
- Evidence of self-harm, or an expressed desire to cause self-harm
- Expressed suicidal thoughts
People experience depression and anxiety differently, and there are also different levels of severity of depression. As soon as you feel that your client is unable to manage symptoms of their own with lifestyle changes, they need to see a specialist. You could be saving their life.

Get Your Free Guide
Learn How to Start a Fulfilling, Impactful Career as a Holistic Health Coach
You’ll learn:
- Why holistic health matters
- If holistic health coaching is right for you
- What career opportunities exist for health coaches
- And more!



